In this Post
- What Leads to Suicidal Ideation?
- Symptoms of Suicidal Ideation
- Ketamine and Suicidal Ideation
- What to Do if It’s Urgent
The definition of suicidal ideation varies across the medical field, posing diagnostic and research challenges to health professionals. It is often referred to as suicidal thoughts or ideas and sometimes includes suicidal planning. Due to the varying definitions, the spectrum of suicidal ideation could be anything from wishing to fall asleep and never wake up to an obsession with self-destruction.
One drastic issue lies in how we measure suicidal ideation. “Have you ever seriously considered suicide?” generates different responses than asking, “have you had fleeting thoughts of suicide?” The bottom line is that there is no consistent operational definition for suicidal ideation, but it is widely agreed that suicidal ideation involves some thought or intention to end one’s life
What Leads to Suicidal Ideation?
The American Foundation for Suicide Prevention reports no singular cause for suicide. One may struggle with mental health problems like depression, substance abuse, bipolar disorder, schizophrenia, brain injuries, or more. Environmental factors may also play a role, with access to firearms and drugs, prolonged stress, stressful life events like divorce or financial crisis, or exposure to another’s suicide possibly heightening an individual’s risk factor.

Symptoms of Suicidal Ideation
Common behaviors related to suicidality are:
- Increased use of harmful substances
- Researching how to end one’s life
- Social withdrawal
- Drastic changes in sleep schedule
- Visiting/calling people to say goodbye
- Giving away possessions
- Aggression or fatigue
Likewise, suicidal ideation often shows itself as changes in mood. Typically, it surfaces through illnesses like depression, anxiety, loss of interest, irritability, humiliation or shame, agitation or anger, or relief 3.
Suppose you or a loved one experiences any of the signs above or begins talking about self-harm, hopelessness, having no reason to live, being a burden to others, or feeling trapped. Treatment for suicidal ideation varies from person to person, so immediate action is crucial, and a medical professional should be contacted immediately.
Ketamine and Suicidal Ideation
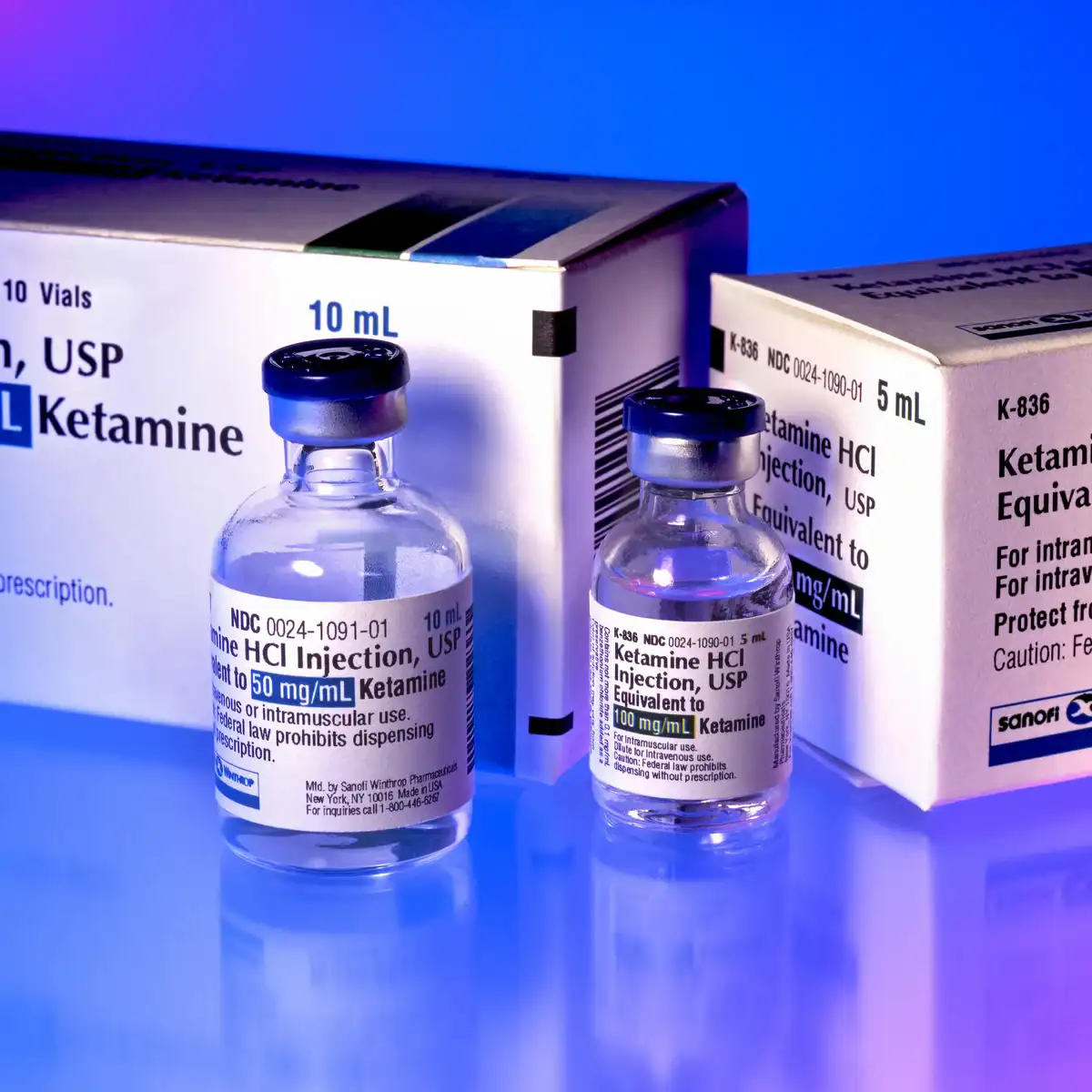
While treatment types vary by person, a suitable option may be intravenous ketamine infusions. One study examined ketamine infusions for patients with treatment-resistant depression (TRD) and suicidality. It assessed 26 patients with TRD using the suicidality item of the Montgomery-Asberg Depression Rating Scale two hours before and 24 hours after intravenous ketamine infusions. The findings showcased ketamine’s rapid beneficial effects for those patients while also pointing toward the need for further studies 4.
Another systematic study of ketamine as a potential treatment found studies detailing a “rapid and clinically significant reduction,” with the results aligning with previously described data on ketamine and TRD. The review found that ketamine’s rapid effects positively reduce depressive symptoms (and suicidality) with few short-term side effects 5.
Finally, a study of 49 emergency room patients with suicidal intentions, with or without unsuccessful attempts, discovered conflicting results to the ones above. It found that patients given 0.2mg/kg of ketamine did not experience a significant reduction in suicidal ideation. In a follow-up ten days after infusion, researchers found that some patients still had suicidal ideations. This could be, they theorized, due to the low dose of ketamine. Indeed larger doses are provided in most clinics, including at Avesta, as research has shown that doses of 0.5mg/kg or greater are much more beneficial, as seen in the studies above.
What to Do if It’s Urgent
The American Foundation for Suicide Prevention has resources available if you or someone you love are considering suicide. You can call the National Suicide Prevention Lifeline 24/7 at 800-273-8255. Or you can text anywhere within the United States by contacting the Crisis Text Line at any time, text HOME to 741741.
Our Mission
At Avesta Ketamine & Wellness, our mission is to help patients optimize their mental and physical wellness through our many high-end infusion options. We offer treatments for mood disorders, depression, anxiety, PTSD, pain management, and more. To schedule a consultation, either call our office or go online to book a visit today at any of our 3 convenient locations in the DC Metro area.

Footnote References:
1 Harmer, B., Lee, S., Duong, T. vi H., & Saadabadi, A. (2022). Suicidal ideation. In StatPearls. StatPearls Publishing. http://www.ncbi.nlm.nih.gov/books/NBK565877/
2 Berman, A. L., & Silverman, M. M. (2017). How to ask about suicide? A question in need of an empirical answer. Crisis, 38(4), 213–216. https://doi.org/10.1027/0227-5910/a000501
3 Risk factors, protective factors, and warning signs. (2019, December 25). American Foundation for Suicide Prevention. https://afsp.org/risk-factors-protective-factors-and-warning-signs/
4 Price, R. B., Nock, M. K., Charney, D. S., & Mathew, S. J. (2009). Effects of intravenous ketamine on explicit and implicit measures of suicidality in treatment-resistant depression. Biological Psychiatry, 66(5), 522–526. https://doi.org/10.1016/j.biopsych.2009.04.029
5 Reinstatler, L., & Youssef, N. A. (2015). Ketamine as a potential treatment for suicidal ideation: A systematic review of the literature. Drugs in R&D, 15(1), 37–43. https://doi.org/10.1007/s40268-015-0081-0
6 Kashani, P., Yousefian, S., Amini, A., Heidari, K., Younesian, S., & Hatamabadi, H. R. (2014). The effect of intravenous ketamine in suicidal ideation of emergency department patients. Emergency (Tehran, Iran), 2(1), 36–39.
Other References:
Avesta ketamine and wellness: Anesthesiology: Mclean, va, bethesda, md & washington, dc. (n.d.). Retrieved September 22, 2022, from https://www.avestaketaminewellness.com/services
Suicide and suicidal thoughts—Diagnosis and treatment—Mayo Clinic. (n.d.). Retrieved September 22, 2022, from https://www.mayoclinic.org/diseases-conditions/suicide/diagnosis-treatment/drc-20378054
Photo by Karolina Grabowska from Pexels: https://www.pexels.com/photo/woman-comforting-her-worried-partner-6134922/
Author Dr. Ladan Eshkevari, PhD, CRNA, FAAN Dr. Eshkevari is the lead clinician at Avesta, and is a long time researcher and educator in physiology, biophysics, and anesthesiology. She is passionate about assisting patients with retractable, difficult to treat mood disorders, and relies on the latest research to bring evidence to Avesta’s practice to better understand and serve patients.