In this Post
- Is Ketamine Therapy Addictive?
- Historical Context of Ketamine Use
- Ketamine’s Addictive Potential Compared to Other Substances
- Ketamine, Addiction, and Monitored Treatment
- Avesta Ketamine Therapy for Substance Use Disorders
Is Ketamine Therapy Addictive?
Decades of clinical evidence show that ketamine’s therapeutic potential far exceeds its traditional uses in anesthesia and acute pain management. A dissociative compound, ketamine can also effectively relieve chronic pain and treatment-resistant mental health conditions like depression, suicidality, and PTSD.
Like any drug, ketamine can lead to misuse and dependence when used nonmedically. However, monitored ketamine therapy in clinical settings does not come with the same addiction risks. On the contrary, ketamine therapy can be beneficial for people with alcohol and substance use disorders.
This article delves into ketamine’s paradoxical nature, exploring its addictive potential alongside its emerging role in treating mental health and substance use disorders.
Ketamine’s Historical Context

Ketamine was first developed in the 1960s by Calvin L. Stevens at Parke-Davis Pharmaceutical Company as an alternative to anesthetics that caused respiratory depression.
In 1964, researchers used ketamine in humans for the first time, and it quickly became the preferred anesthetic for battlefield medicine. Veterinarians also discovered ketamine’s usefulness and continue to employ it today.
By the mid-1960s, people also began using ketamine recreationally. Users found the drug appealing because of its psychoactive effects, including dissociation, euphoria, and hallucinations, depending on the dose and the person. By the late 1970s, ketamine flooded the streets under various names, including Vitamin K, Special K, KitGreen, Purple, Mauve, Special LA, and Super C, and government agencies reported its abuse potential.
Concurrently, clinicians utilizing ketamine for anesthesia began observing exciting effects in their patients. Patients regularly reported improved mood following procedures, piquing the interest of psychiatrists and researchers. In the early 2000s, scientists began investigating ketamine for its potential mental health benefits.
Since then, various studies have uncovered ketamine’s ability to rapidly improve:
- Depression
- Post-traumatic stress disorder (PTSD)
- Chronic pain
- Obsessive-compulsive disorder (OCD)
- Bipolar disorder
Ketamine’s diverse history makes it nuanced as both a medical marvel and a potential recreational hazard.
Ketamine’s Addictive Potential Compared to Other Substances
The FDA classifies ketamine as a Schedule III drug, signifying a perception of moderate to low dependence potential and recognized medical uses. Despite this status, many experts do not consider ketamine physiologically addictive, and literature indicates it has a much lower abuse potential than most legal drugs and pharmaceuticals.
Ketamine vs alcohol
Take alcohol, for example. This culturally accepted drug is fully legal and unscheduled. However, alcohol is addictive and can be extremely dangerous. According to the 2021 National Survey on Drug Use and Health (NSDUH), 29.5 million people ages 12 and older (10.6%) had alcohol use disorder (AUD) in the past year.
Comparatively, scientific literature has identified fewer than 15 cases of ketamine dependence over the past 20 years. Admittedly, there may be many unreported incidences in the population. Still, ketamine dependence is much rarer than alcohol abuse.
Additionally, ketamine can be used to treat substance use disorders, including alcohol addiction.
According to a recent study, combining low-dose ketamine with psychological therapy for AUD significantly extended sobriety compared to the control groups. Patients receiving ketamine and therapy averaged 162 abstinent days out of 180 in the six-month follow-up period. They were 2.5 times more likely to remain completely abstinent at the trial’s end than the placebo group.
Ketamine vs nicotine
Nicotine is also unscheduled and fully legal, yet highly addictive. Nicotine in cigarettes exerts rewarding effects by activating nicotinic acetylcholine receptors (nAChRs), making smoking cessation challenging.
Comparatively, ketamine does not primarily act on the brain’s reward pathways, which reduces its potential for addiction. Instead, ketamine blocks NMDA receptors in the brain’s glutamatergic system, leading to changes in synaptic plasticity, which can affect mood and perception. This action contributes to its rapid antidepressant effects.
A recent study investigated ketamine’s ability to reduce nicotine addiction in rats. Researchers hypothesized that ketamine could disrupt the neural pathways associated with dependence due to its NMDA action.
The team administered sub-anesthetic doses to addicted rats, observing a significant reduction in nicotine self-administration. The outcomes were dose-dependent, with higher ketamine amounts leading to greater reductions in nicotine intake.
Ketamine vs morphine
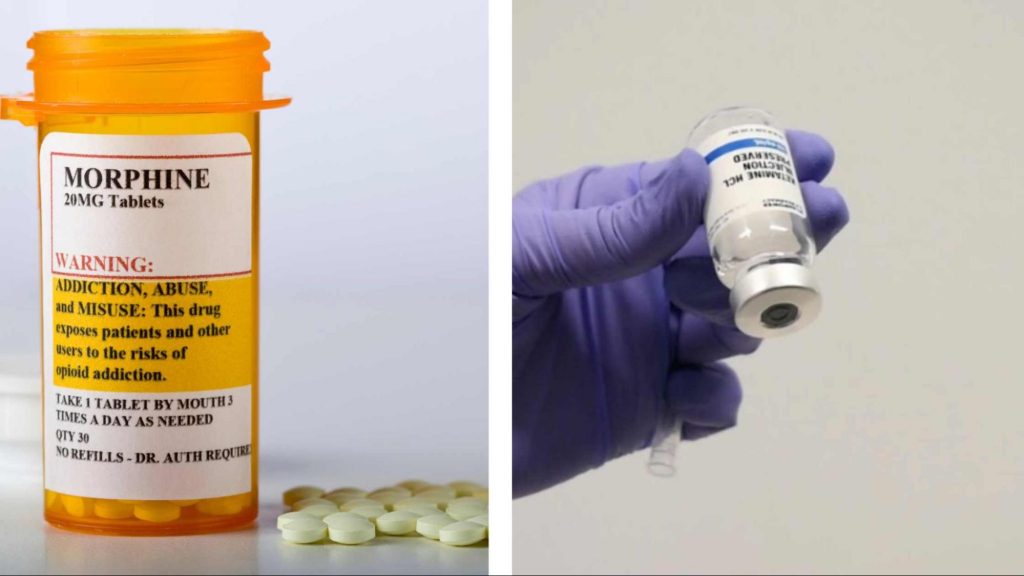
Morphine is an opioid pain medication, highly effective for treating severe pain but notorious for its high addictive potential. Its addiction risk stems from its euphoric effects and the way it activates opioid receptors in the brain, altering pain perception and emotional responses.
Morphine’s effects often lead to tolerance, necessitating higher doses for the same effect. In the United States, the National Institute on Drug Abuse reports that “up to 50% of patients on chronic opioid therapy meet the criteria for opioid use disorder.”
Ketamine, by contrast, acts as an NMDA receptor antagonist, a different mechanism from opioids. This action makes ketamine less likely to trigger abuse and dependence.
Interestingly, scientists have also discovered that ketamine can help people with opioid addiction. Some clinicians are administering ketamine in conjunction with buprenorphine (Suboxone), one of the two FDA-approved medications for opioid use disorder. Other doctors use ketamine to help manage opioid withdrawal symptoms, potentially facilitating a reduction in opioid use.
Ketamine vs Benzodiazepines
Benzodiazepines are widely prescribed for anxiety, insomnia, and seizure disorders, acting as central nervous system depressants. They promote sedation and muscle relaxation by enhancing the effect of the neurotransmitter GABA,
Schedule IV substances in the U.S., benzodiazepines, have a lower perceived abuse potential than Schedule II or III drugs. However, long-term and recreational use can lead to tolerance, dependence, and withdrawal symptoms. From 2015 to 2019, an estimated 17.7% of all people who used benzodiazepines in the United States reportedly misused them.
By contrast, recreational ketamine use in the United States is relatively low, with less than 1% of Americans engaging in it.
Researchers are also investigating ketamine as a treatment option for severe benzodiazepine withdrawal.
Ketamine, Addiction, and Monitored Treatment
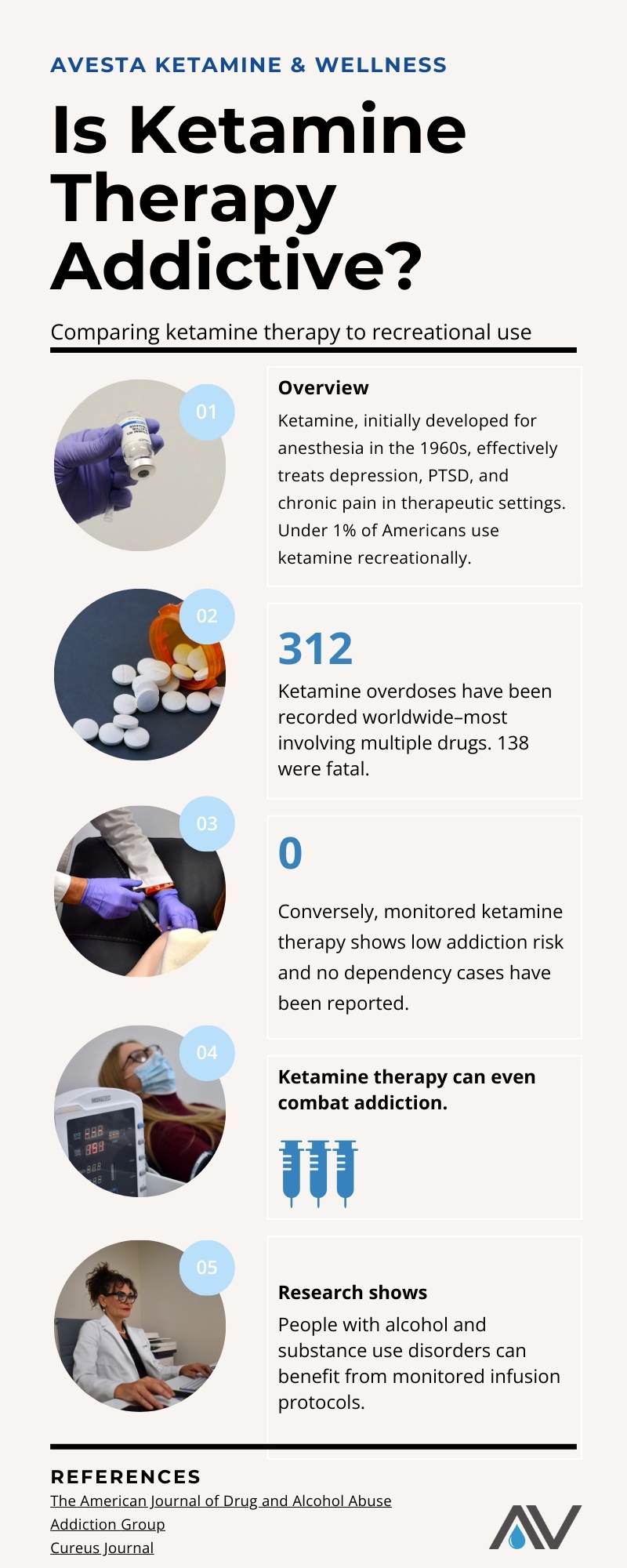
Researchers recently investigated ketamine’s addiction and safety risks, comparing recreational misuse to ketamine therapy.
The team conducted electronic searches across three databases for all ketamine-related overdoses and deaths leading up to 2019. They examined 34 articles, with 18 reporting fatal cases and 16 detailing overdoses, predominantly in males aged 2 to 65 years. 312 overdoses occurred, and 138 people died.
The study highlighted that 53% of the reported cases involved poly-substance use, with ketamine being the dominant in most.
Significantly, no overdoses or deaths were linked to the therapeutic use of ketamine as an antidepressant. The study deduced that while the recreational use of ketamine and its analogs poses serious risks, medicinal applications are safe and even essential, according to the World Health Organization.
The authors concluded by advising ketamine clinics, like Avesta, to remain vigilant, balancing these risks against the compound’s therapeutic benefits.
Avesta’s ketamine clinics in Virginia, D.C., and Maryland have served over 1000 patients without safety issues or addiction occurrences following treatment. Its care team believes that low, controlled doses in a monitored environment over a defined period reduce the chances of addiction.
Avesta Ketamine Therapy for Substance Use Disorders

Substance abuse disorder patients seeking ketamine in Maryland, Virginia, or D.C. can absolutely benefit from Avesta’s infusion therapy protocols. Avesta takes a collaborative approach to caring for these clients.
In substance abuse cases, Avesta practitioners partner with the patients’ psychiatrists and primary care physicians to formulate a safe and effective treatment plan. The team only administers in-office infusions and does not prescribe at-home ketamine sprays or lozenges.
The Bottom Line
Ketamine is a potent therapeutic with dangerous potential. However, it exhibits a lower risk of addiction and dependence in medical settings like Avesta’s. Practitioners at Avesta ensure precise, individualized treatment, reducing the risk profile. Patients with concerns, especially those with a personal or family history of addictions, should contact Avesta’s ketamine clinics for more information and clarification.