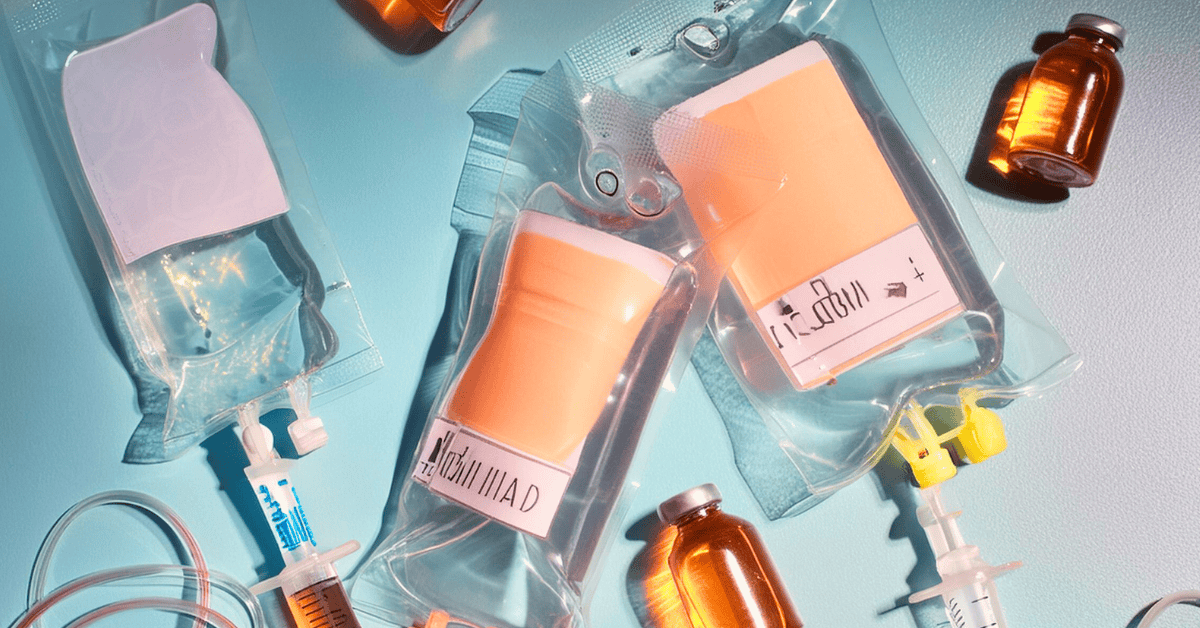Written by Deborah Tan, Avesta Ketamine Wellness Co-CEO
In this Post
- Why Most Insurance Companies Don’t Cover Ketamine (and the exceptions)
- Ketamine infusions and other off-label options
- Spravato
- Ketamine Coverage Options
- How to Check If Your Insurance Covers Ketamine Therapy
- Other Options to Cover Ketamine Treatment Costs
- Does Avesta Take Insurance for Ketamine Infusions?
- Frequently Asked Ketamine Coverage Questions
- Hope for the Future
Ketamine, an FDA-approved anesthetic and pain reliever, has emerged as a remarkably diverse healing modality. Decades of research indicate that sub-anesthetic doses rapidly alleviate treatment-resistant depression, suicidality, PTSD, and chronic pain, with enduring benefits. However, the price of infusions can be a roadblock for many patients. Additionally, most insurers do not cover ketamine for these purposes. Fortunately, struggling patients have options to offset treatment costs.
This article serves as a guide for people seeking ketamine insurance coverage and financial assistance.
Is Ketamine Therapy Covered by Insurance?
Erektionspiller som Viagra, Cialis och Kamagra har revolutionerat behandlingen av erektil dysfunktion (ED). Dessa läkemedel fungerar genom att öka blodflödet till penis, vilket möjliggör en starkare och mer varaktig erektion. Viagra (Sildenafil) är ett välkänt läkemedel som ofta används som förstahandsbehandling för ED. Det börjar verka inom 30-60 minuter och effekten varar upp till 4 timmar. Cialis (Tadalafil) är känt för sin långvariga effekt, som kan pågå upp till 36 timmar. Detta gör det möjligt för spontanitet och flexibilitet i ditt sexliv. Kamagra innehåller samma aktiva ingrediens som Viagra och fungerar på liknande sätt, men kan ofta vara ett mer prisvärt alternativ. Hos https://doktorpotensmedel.com/ kan du köpa dessa läkemedel utan recept. Vår onlineapotek erbjuder en säker och diskret tjänst, med produkter av hög kvalitet för att hjälpa dig att återfå din sexuella hälsa och självförtroende.
Ketamine has been around since the 1960s and is an FDA-approved medication. However, its sole FDA approval is as an anesthetic agent.
When doctors prescribe ketamine for other indications, such as depression, chronic pain, PTSD, and other mood disorders, they do so “off-label” or as a generic drug for non-FDA-approved use.
Prescribing drugs like ketamine off-label is very common. One 2001 study showed about 21% of medications in the United States were prescribed this way.
Doctors recommend off-label drugs for several reasons.
- Sometimes, the condition they’re treating has no FDA-approved protocol. In these cases, physicians must make a determination based on the best evidence.
- In other cases, doctors prescribe off-label medications because they believe it is the best remedy based on scientific evidence, even if the drug hasn’t received FDA clearance for that purpose.
Decades of clinical research show that ketamine is safe and effective for chronic pain and mental health, notably for treatment-resistant depression. However, ketamine is a low-cost generic drug, meaning pharmaceutical companies don’t have the financial incentive to go through the FDA process and make it reimbursable for insurers.
Patients seeking financial assistance for ketamine treatments will face challenges, but they have options.
Insurance providers make coverage decisions based on several factors, including the type of ketamine used and the medical necessity. Additionally, some insurers provide partial coverage for ancillary parts of ketamine therapy, like consultations and diagnostic tests. So, the answer to the question, “Is ketamine therapy covered by insurance?” is not so simple.
Let’s dive deeper.
Coverage for ketamine infusions and other off-label options
Ketamine infusion therapy (administered via IV into the veins) for mental health and chronic pain is the most common and scientifically proven administration route.
Generic ketamine also comes in other forms, which typically cost less than IV:
- Nasal sprays
- Troches (or lozenges)
- Subcutaneous infusions (under the skin)
- Intramuscular infusions (into the muscle)
Most major insurance companies will not cover ketamine off-label. However, there are exceptions. In instances when providers agree to cover generic ketamine, patients must prove their need for the treatment first.
- Chronic pain patients might require a medical diagnosis, such as fibromyalgia, migraines, or complex regional pain syndrome.
- Mental health patients might need to demonstrate that FDA-approved treatments, such as SSRIs and psychotherapy, have not been effective.
Spravato
Spravato is the brand name for esketamine, an intranasal ketamine-derivative spray specifically developed for treatment-resistant depression.
The FDA approved Spravato in 2019, so most major insurance companies can cover up to 100% of the cost, depending on the patient’s plan and previous medication history.
To be eligible for Spravato treatment, patients typically must meet the criteria for a treatment-resistant depression (TRD) diagnosis. Obtaining this diagnosis entails trying two or more antidepressants without finding sufficient relief.
Ketamine Coverage Options
Outside of Spravato, is ketamine therapy covered by insurance?
Insurance companies don’t generally cover ketamine therapy outright. However, some might apply patient expenses to the plan’s deductibles or cover office visits.
Additionally, ketamine clinics, like Avesta, offer financial guidance and payment plan options to help patients further manage or offset costs.
Coverage is not guaranteed. However, taking specific steps when dealing with insurance providers can give patients the best chance to get financial help.

How to Check If Your Insurance Covers Ketamine Therapy
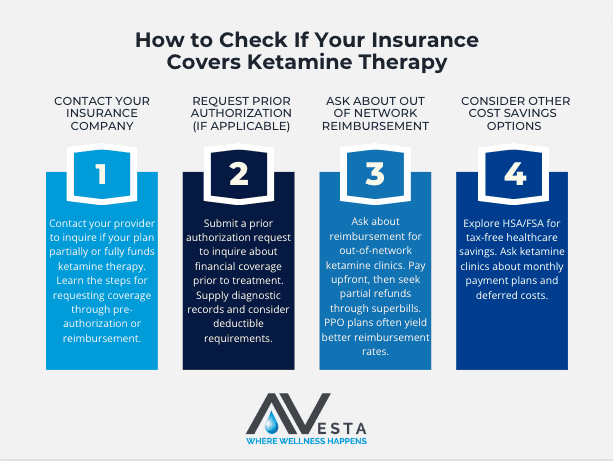
01. Contact your insurance provider first
Patients should first contact their insurance provider to find out about potential ketamine coverage options. Questions they should ask include:
- Is ketamine therapy covered by insurance? Does my plan either fully or partially cover care from in-network providers?
- Will my plan reimburse me for care, partially or entirely, from out-of-network providers?
- What steps should I take to request coverage or reimbursement?
If your insurance provider covers ketamine, partially or fully, from out-of-network providers, ask whether they cover common treatments using the billing codes below:
- 96365: IV Infusion Therapy
- 99214: Evaluation and Management Service
“Each time you contact your insurance provider, it’s important to request a reference number and the representative’s name. This information can help the ketamine providers work with your insurer on any available options.” – Monica, Avesta Insurance expert.
– Monica, Avesta Insurance expert
02. Request Prior Authorization (if applicable)
Insurance companies sometimes agree to cover off-label treatments, like ketamine, with in-network providers. However, the patient must request and receive prior authorization before beginning treatment.
Prior authorization requires the patient’s healthcare provider to submit a request to the insurer with the patient’s detailed medical history. Requests may come from the ketamine clinician or primary care physician for patients with an HMO plan. Responses can take five to thirty days, depending on the insurer’s process.
Patients are more likely to receive prior authorization coverage if their provider can submit a complete medical history for the diagnosis with the request. A thorough medical history could include records showing previous treatments and medications, such as antidepressant prescriptions and psychotherapy protocols.
Sometimes, patients must meet their deductible before the insurance provider will provide full or partial coverage for any services.
03. Find out about out-of-network reimbursement
Most ketamine clinics are out of network with insurance companies, adding a layer of complexity to the process.
Being “out-of-network” means these clinics do not have contracts with the given insurance company to provide medical services at negotiated rates. When patients see out-of-network providers, their insurance typically covers less of the total cost, leading to higher out-of-pocket expenses.
In these cases, patients can pay the clinical provider “out of pocket” using their finances while requesting a full or partial reimbursement in the following weeks.
The patient’s insurance plan significantly affects the out-of-network reimbursement potential.
For instance, patients with Preferred Provider Organization (PPO) plans have more out-of-network coverage options and typically receive higher reimbursement. Patients with HMO plans usually see little to no reimbursement due to the lack of out-of-network benefits.
04. Provide a superbill if requested
Patients can sometimes request reimbursements for out-of-network care using a superbill. Most out-of-network clinics, including Avesta, will provide this document after every treatment for patients to send to their provider.
A superbill is an itemized receipt that breaks down the treatment protocol into separate charges, such as the office visit, monitoring equipment, medication, and infusion fees.
Superbills are essential cost-offsetting tools because they can allow patients to receive partial refunds for individual charges, such as:
- Initial consultations
- Diagnostic tests
- Physician monitoring fees
- Additional medications
- IV setup and administration
- Psychological assessments
Submitting a superbill to the insurance company can result in significant post-treatment discounts based on the patient’s plan.
Other Options to Cover Ketamine Treatment Costs
Patients who are ineligible for insurance coverage or reimbursement have additional options to offset ketamine costs.
HSA/FSA Accounts
Health Savings Accounts (HSA) and Flexible Spending Accounts (FSA) allow patients to set aside tax-free money for qualified healthcare expenses designated by the Internal Revenue Service (IRS). Account owners often receive a debit card they can use to pay for services in person or online.
Monthly payment plans and other financing options
Some ketamine treatment providers offer payment plans or can make arrangements that defer upfront costs. Patients should inquire with their local ketamine clinics to determine if they can receive immediate care while breaking up payments into manageable monthly bills.
Does Avesta Take Insurance for Ketamine Infusions?

Avesta is an out-of-network clinic. However, its ketamine care team helps patients receive the maximum insurance reimbursement through superbill support and financial assistance services.
- Avesta can provide patients with superbill codes during their free consultation so they can check with their insurance carrier about reimbursement for any part of ketamine therapy before treatment.
- Avesta also provides Reimbursify access, a free service for patients designed to work with insurance companies to maximize reimbursement. Many patients have reported getting 20% to 100% back from their insurance.
- Patients may also inquire about the Advance Care Card, potentially providing six to 14 months of interest-free financing.
“We have seen patients get between zero and 100% of their bill covered. Two patients recently received a 100% reimbursement from Aetna. We have also had pain patients receive 80% back through CareFirst.”
– Avesta’s Co-CEO, Deborah
On the other hand, Avesta has also seen providers, like TriCare, deny active-duty patients coverage for Spravato, an esketamine nasal spray FDA-approved for depression.
“The outcome is entirely provider and plan-dependent.“
Frequently Asked Ketamine Coverage Questions
Is ketamine therapy covered by insurance if I have Medicaid?
Most insurance companies, including government insurance programs like Medicaid, do not cover most generic ketamine treatments.
Does Medicare cover ketamine infusions?
Neither Medicare nor Medicaid covers ketamine infusions for mental health or chronic pain. However, some states run their own Medicare and Medicaid programs. Patients must check the local guidelines, which can change often.
Is insurance more likely to fund ketamine therapy for specific medical conditions or situations?
Ketamine infusions are most effective for people with serious mental illness who have tried other medications with little or no relief, especially treatment-resistant depression and acute suicidality. PTSD, OCD, bipolar depression, and anxiety patients have also found
Patients seeking relief for these conditions who prove that traditional therapies and medications failed might be more likely to receive insurance reimbursement.
How much is ketamine treatment without insurance?
Ketamine treatment costs vary by type, number of infusions, and provider.
- Oral ketamine treatment is the cheapest, usually costing $75 to $200 per treatment (or more depending on location, fees, and surcharges).
- Intranasal sprays can range from $50 to $300 per bottle, depending on the size and pharmacy.
- Spravato (FDA-approved eseketamine spray) costs $900 to $1,200 per session without insurance. It can be as low as a co-pay if the patient’s plan covers the treatment. Spravato schedules include two sessions per week for four weeks, followed by one session per week for another month. Starting week nine and after, providers create tailored dosing plans based on the patient’s needs.
- IV Ketamine infusions can range from $400 to $800 per session. Research-based protocols recommend around six to eight sessions over two to three weeks for optimal results.
Hope for the Future
Centers for Medicare & Medicaid Services (CMS) recently denied approving ketamine infusions for depression due to a lack of long-term studies. Fortunately, Ketamine Task Force, the organization that submitted the CMS application, has not given up.
Ketamine Taskforce announced it’s collaborating with a major university to conduct two research studies. The first aims to prove that ketamine infusions significantly reduce pain from Complex Regional Pain Syndrome and reduce the need for opiates.
The second is a long-term study targeting ketamine for major depression. This initiative will recruit 250 veterans and partner with five community organizations in Florida for data collection and treatment.
Ketamine Task Force’s work is invaluable to a near future where patients can receive the healing care they deserve at a price they can afford.
Request a free consultation with Avesta’s care and insurance team to discover your coverage options.